It is estimated that approximately 110,000 heat -related deaths in Europe during the summer in 2022 and 2023 combined1. This is almost the same as if it was a fully occupied jumbo plane every day for 16 weeks. Meanwhile, a wide range of heat -related effects disrupts people’s lives. Hot weather increases mental health problems2It increases the possibility of violence3 And it makes pregnant women more likely to give birth prematurely4. In the classroom, it weakens the ability of children to learn5.
The shade is a basic solution for the hottest cities
The problems are expected to become much worse. Without better adaptation, it is expected that the deaths associated with the heat will rise 3.7 times by the middle of the century if global temperatures reach 2 degrees Celsius higher than pre -industry levels6. (In 2024, the average global temperature exceeded 1.5 ° C above the pre -industrial levels for the first time) In the lost productivity by 2030.
Currently, most methods that alert the public to heat health around the world use the surrounding temperature sills (air) to stimulate warnings-usually wide recommendations to reduce activity, survival wet, etc. These thresholds generally depend on comprehensive statistical connections between the surrounding temperatures and regional increases in death and disease7. But thermal stress is defined by more than just a temperature, and it can affect multiple physiological systems, including the heart and kidneys4. The risk of individuals varies greatly, depends on factors such as their age, the health of their kidneys and their heart, what they wear and the level of their activity.
Two of us (OJ and FT) experiment with the combination of physiological models and weather data to estimate the “thermal health risk” of people. We believe that thermal adaptation can be promoted significantly using an approach based on physiology that focuses on hot people, rather than just hot weather.
How hot is very hot?
Most people can carry basic body temperatures safely up to about 39 ° C. If the body temperature exceeds this value, the risk of exhausting heat increases, with symptoms, including nausea, dizziness and vomiting. At basic temperatures above 40 ° C, the heat blow can occur. Here, increasing the permeability of the intestine, caused by low blood oxygen delivery, allows toxic molecules associated with some bacteria to leak into the bloodstream. This can lead to an inflammatory response that infiltrates the cause4.

Water sprinklers from a crane to help calm construction workers in Nanjing, China, during high temperatures last month.Credit: Liu Jianhua/Vcg via Getty
Whether anyone affected by hot weather depends on a mixture of environmental factors and characteristics of this individual. In addition to the air temperature, three important thermal environments features: radiation, humidity and wind speed8. Someone in direct sunlight can be exposed to radioactive temperatures, meaning more than 20 ° C of shadow temperatures. (The temperatures of the air used to stimulate healthy warnings in the shade are measured. The ability to lose heat is also affected by the evaporation of sweat by thermal properties and evaporation of clothes8And age, body size and some medications9. Even light activity, such as walking, is more than twice the production of internal heat, and thus increases the risk of a person from facing health problems in hot weather.
Thermal regulation of the body is supported by a massive red distribution of the blood to the skin. In hot weather, the need for heat loss increases, which means that to maintain blood pressure, the heart must often pump with greater strength. People with heart disease are less able to compensate for increased pressure, and thus face the risk of cardiovascular4. Blood redistribution can also destroy organs like the kidneys by reducing the amount of oxygen that is delivered to them. The dance blood volume of dehydration in hot weather forces the heart to work harder, and frequent dehydration can contribute to kidney fibrosis (the accumulation of the tissue of the scar in the kidneys) and chronic kidney disease4. People with kidney disease face a greater risk of kidney failure in severe heat.
The physiological approach based on science
When the air temperatures are expected to exceed a specific threshold, warnings that help prepare health and energy systems for severe heat attacks are running1. But health -related warnings are limited to the quality of the data available on deaths and heat -related disease10And it does not allow the exact sewing to protect the groups of greater danger.

Why do we still do not know the increasing health risks of climate change
Also, the narrow focus on air temperature enhances the firm belief that reducing the surrounding temperatures is the only way to reduce the effects of heat on health11. But attempts to do this can be unsustainable or ineffective. Hot surface paint like Ways with reflector coatingFor example, it is likely that it has a little effect on physiological heat stress or even on the perceived discomfort unless people are lying on the ground, and their number of calories may increase on people. The benefit of increasing green areas and tree cover in cities is often evaluated according to their ability Reducing the sidewalks of the sidewalks or average air temperatureAlthough the main thermal benefit of urban green increases people’s arrival to the shade.
In an approach based on physiology, all parameters with high -quality data can be integrated enough in models to estimate three factors: the basic body temperature of the person, the level of dehydration and strain on the heart and blood circulation8. In our experimental studies in Sydney, Australia, we merged six criteria: the surrounding temperature, the level of thermal radiation, the level of humidity, the wind speed, the level of a person’s activity, the thermal properties and evaporation of their clothes. (Physiological acclimatization-well-understood physiological adjustments can also be combined when a person is exposed again and again to a hot environment-.)
The estimates of physiological stress can then be compared to long physiological safety thresholds for various groups, based on properties such as age, whether the person has a pre -existing condition, what medications they take and so on. For example, people with coronary artery disease can tolerate much lower cardiovascular strain than healthy individuals.12Those who suffer from heart failure or kidney disease can tolerate less dehydration. The final combined result is the “thermal health risk” of the individual (see “evaluating the health risks caused by heat using physiology)).
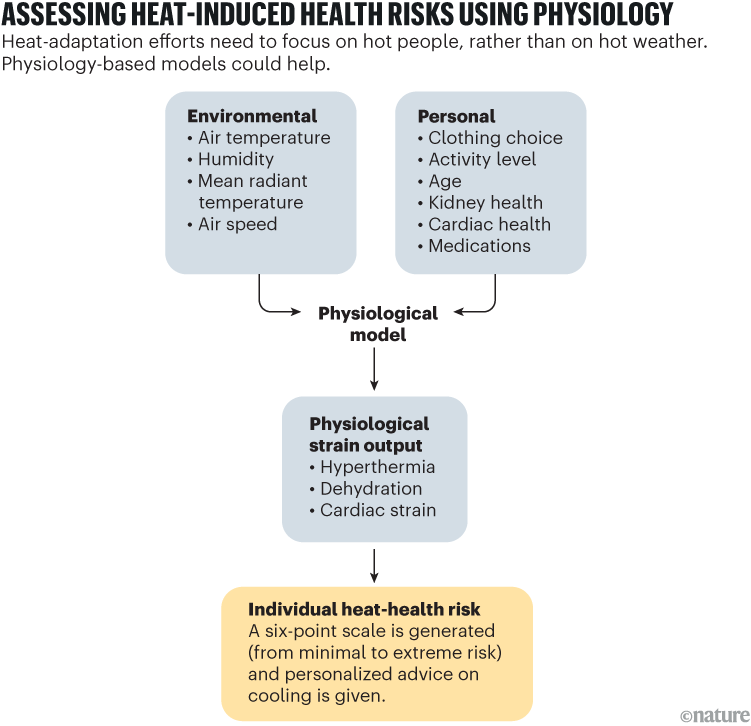
Source: O. Jay And others.
Achieve this
The vital physiological and physical models needed for this type of approach It is already available. To provide individuals with a classified classification of the risk of heat stress that uses a six -point scale, two of us (OJ and FT) developed a free internet tool called Heatwatch (see go.nature.com/44ymweq). This allows users to create personal profiles by providing their age, related health conditions, medications, access to air conditioning, etc. Then it provides a seven -day prediction of thermal health risks and provides a specially designed evidence for each profile.
Ultimately, we plan to develop an online interface similar to information units that follow the risk of infection with the Coronverus SARS-2 virus during the Covid-19 pandemic. Such a façade can allow governments, public health organizations, policy makers and other better expectations of a place and when certain groups will face high temperature health risks. This must take measures to reduce these risks, such as publishing Purifying cooling centers For people who have no shelter, more expensive and cost -effective.

Hospital in New Delhi has a specialized unit for treating people with stroke.Credit: Vipin Kumar/Hindustan Times via Getty
